CASE20220814_002
A Case of Critically Confirmed COVID - 19 in a 52 Year Old Filipino Male Presenting With Multivessel Coronary Artery Disease
By , ,
Presenter
Maria Antonette Bernal Gelindon
Authors
1, 1, 1
Affiliation
, Philippines1
Complex PCI - Multi-Vessel Disease
A Case of Critically Confirmed COVID - 19 in a 52 Year Old Filipino Male Presenting With Multivessel Coronary Artery Disease
1, 1, 1
, Philippines1
Clinical Information
Patient initials or Identifier Number
EG
Relevant Clinical History and Physical Exam
Patient is a known hypertensive and diabetic with prior history of stroke. A day prior to admission, the patient presented with sudden onset of chest pain , non radiating, graded 9/10 in severity accompanied with dyspnea and shortness of breathing hence rushed to the emergency room. Upon arrival he was recieved unstable and drowsy. Work ups done confirmed ST elevation myocardial infarction with posterior involvement and RT PCR for SARS CoV-2 revealed positive.
Relevant Test Results Prior to Catheterization
On arrival, diagnostics were done which include electrocardiogram showing inferior wall infarction with posterior wall involvement .Chest radiograph was also requested which revealed congested lungs and pneumonia. High sensitive troponin I showed elevated value. Complete blood count also showed leukocytosis with neutrophilic predominance. A SARS-CoV 19 swab was done which revealed positive for Covid-19 infection.
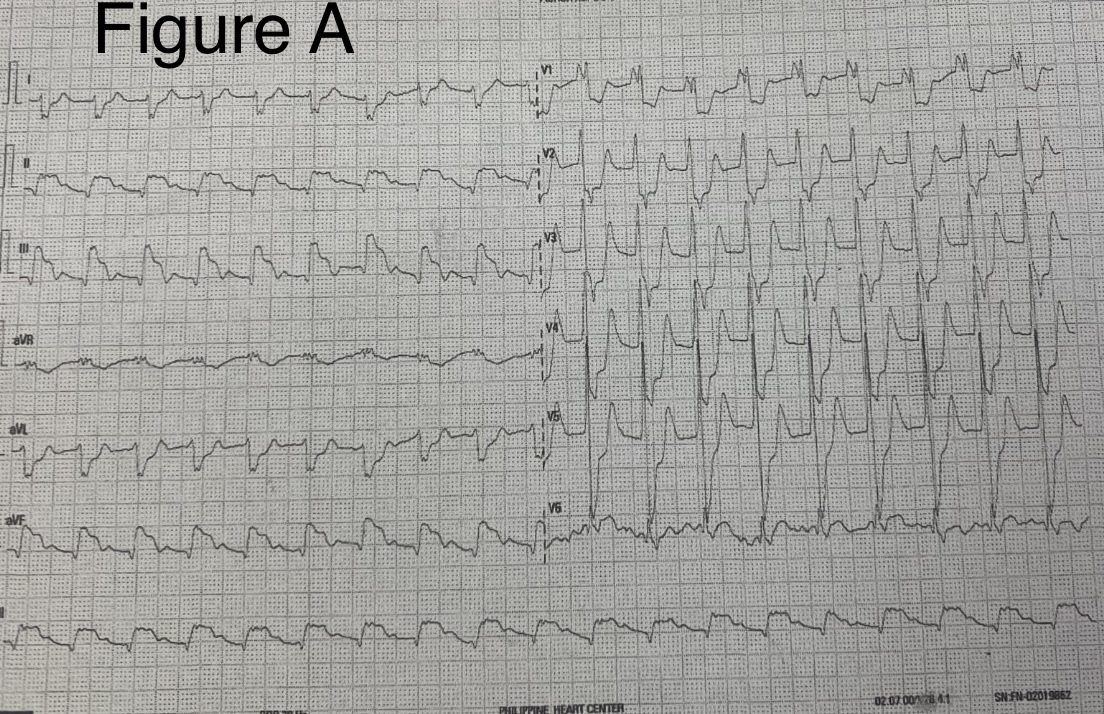
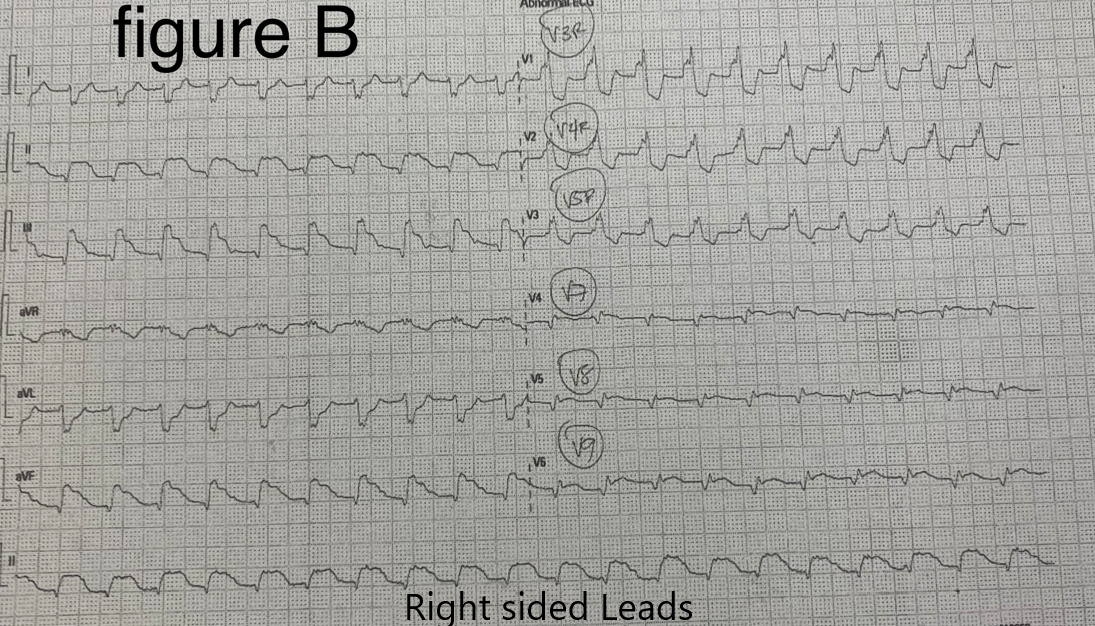
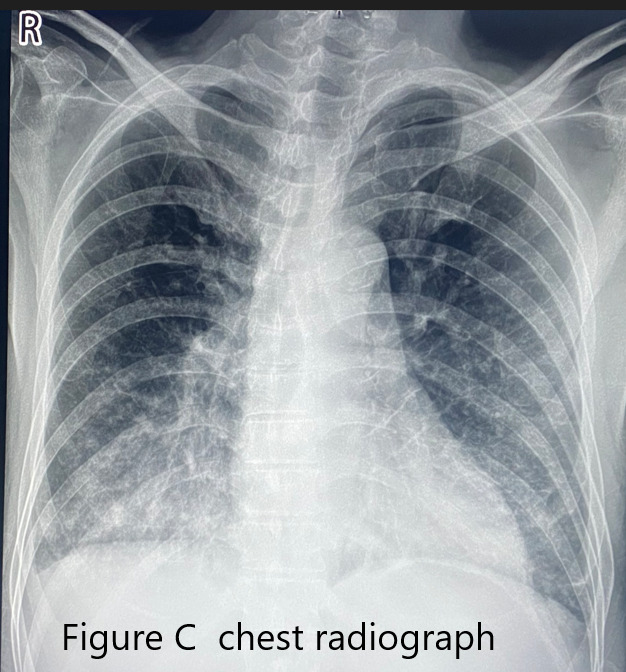



Relevant Catheterization Findings
Left heart catheterization and coronary angiogram were done which showed calcifications .The left main coronary artery showed a fair sized vessel with 70-80% aortoostial stenosis. The left anterior descending artery showed a 95-99% ostioproximal stenosis. The left circumflex artery is totally occluded at the proximal segment and the right coronary artery showed 95% proximal segment stenosis becoming totally occluded at the mid segment .Left ventricular end diastolic pressure is elevated at 40mmHg.
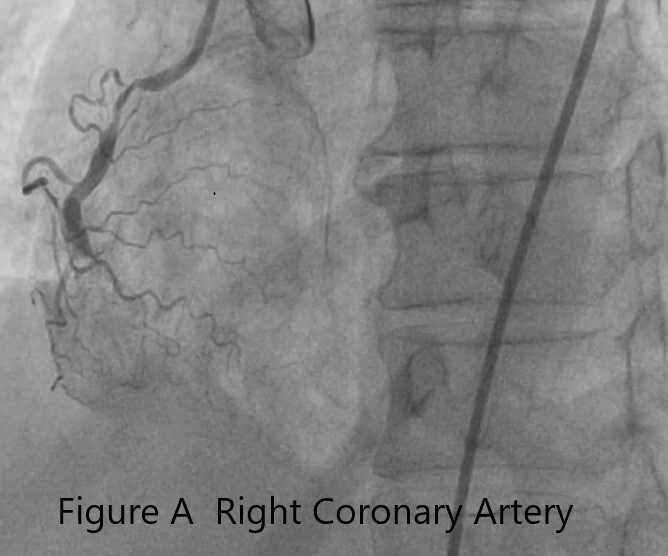
 Video A right coronary artery (2).mp4
Video A right coronary artery (2).mp4
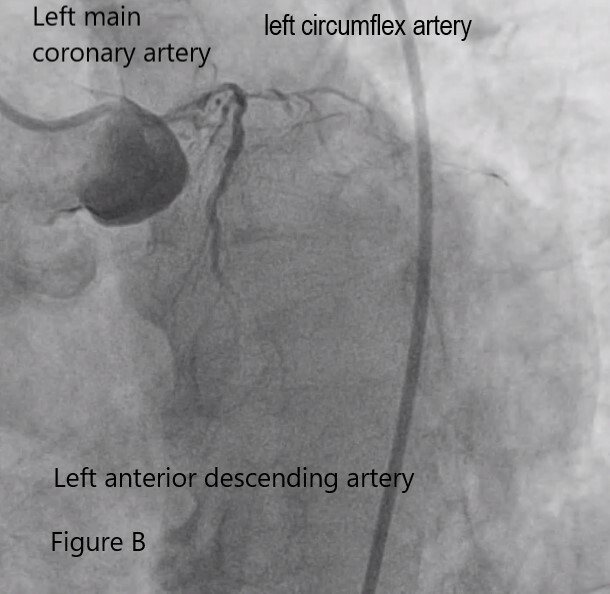
 Video B Left main ,Left anterior descending and left circumflex artery.mp4
Video B Left main ,Left anterior descending and left circumflex artery.mp4
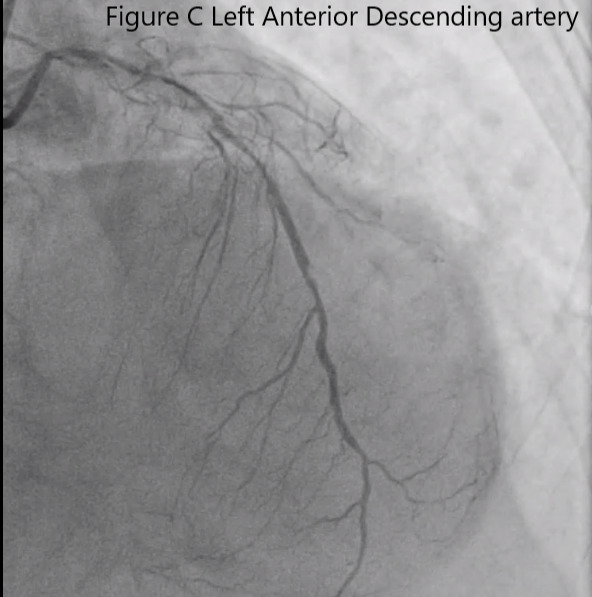
 Video C Left anterior descending artery (2) (2).mp4
Video C Left anterior descending artery (2) (2).mp4



Interventional Management
Procedural Step
Initially, balloon angioplasty of the right coronary artery was done over the culprit lesion. Intraprocedural event noted, he had hypotension and bradycardia hence an intra aortic balloon pump and temporary pacemaker were inserted. Patient was referred to surgery for urgent coronary artery bypass however since patient was positive for COVID -19 infection a 21-day recovery period was recommended prior to operation thus Percutaneous Coronary Intervention was decided by the Heart Team . Percutaneous transluminal coronary angioplasty of the right coronary artery was done and stents were placed at the proximal , proximal to mid and distal right coronary artery. Intravascular ultrasound post stent showed well opposed and expanded right coronary artery. An intravascular ultrasound guided percutaneous intervention of left main and left anterior descending artery was also done. A percutaneous transluminal coronary angioplasty guidewire was advance across the left main coronary artery to proximal left anterior descending artery and noted heavy calcification at proximal left anterior descending artery hence rotational atherectomy was carried out. A guidewire was then advance to the proximal to distal left anterior descending artery and a stents were placed at the left main to proximal left anterior descending artery and proximal to mid left anterior descending artery. Intravascular ultrasound post stent showed well opposed and expanded proximal to mid left anterior descending artery.
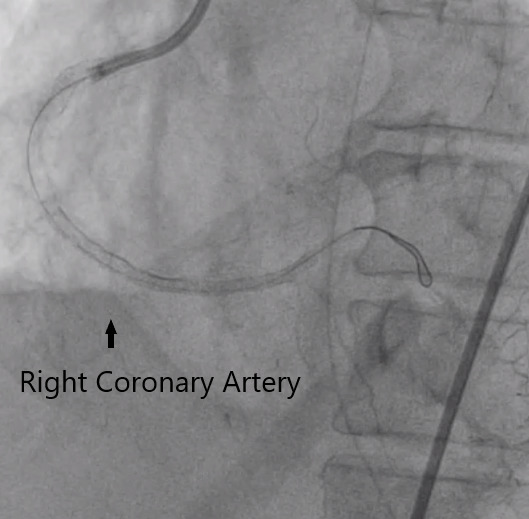
 Video A right coronary artery (1).mp4
Video A right coronary artery (1).mp4
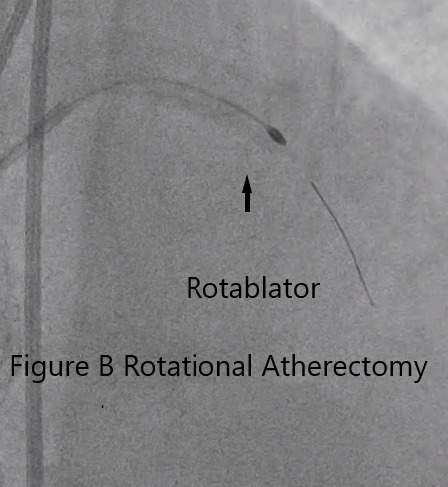
 Video B rotational atherotomy (3) (1).mp4
Video B rotational atherotomy (3) (1).mp4
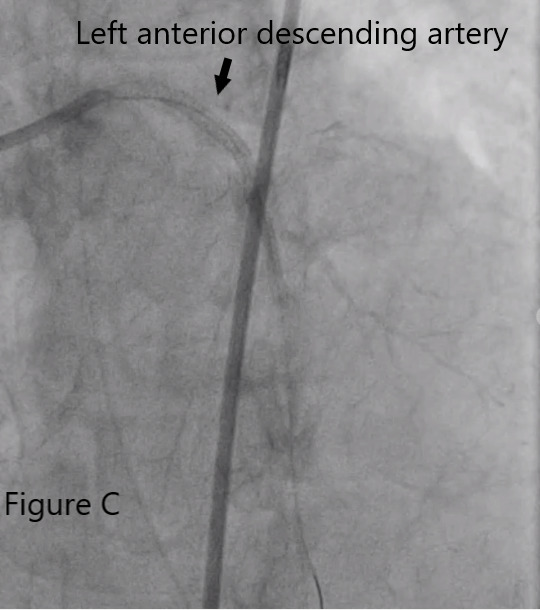
 Video C Left anterior descending artery .mp4
Video C Left anterior descending artery .mp4



Case Summary
Covid-19 pandemic has affected the standard of care on managing acute coronary syndrome . Patients with COVID -19 infection have an overwhelming inflammatory and catabolic state therefore the recommendation for urgent coronary artery bypass cannot be done hence exploring complex procedure applying rotational atherectomy plus intravascular ultrasound technique is a favorable option for this complex case with multiple comorbidities and multivessel coronary artery disease involvement . Given the urgency in this case the team has successfully revascularized the patient and weaned off from mechanical ventilatory and medical support.
